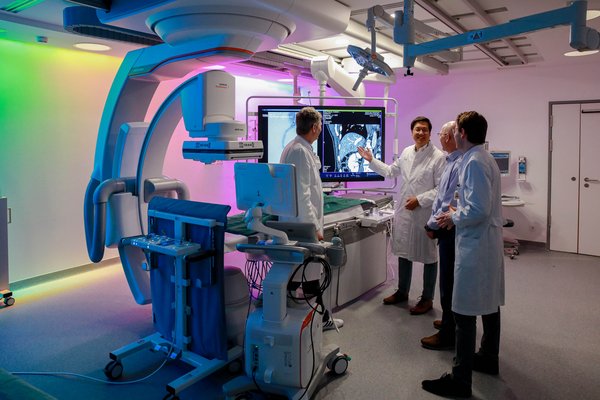
Unsere Behandlungen im Überblick
 Atemwege
Atemwege Augen
Augen Brust (Frau)
Brust (Frau) Geburt und Schwangerschaft
Geburt und Schwangerschaft Geschlechtsorgane (Frau/Mädchen)
Geschlechtsorgane (Frau/Mädchen) Weitere
Weitere Geschlechtsorgane (Mann/Junge)
Geschlechtsorgane (Mann/Junge) Hals, Nase, Ohren
Hals, Nase, Ohren Hand und Fuß
Hand und Fuß Haut und Haare
Haut und Haare Herz, Blutgefäße, Kreislauf, Blut
Herz, Blutgefäße, Kreislauf, Blut Infektionskrankheiten
Infektionskrankheiten Kinder und Jugendliche
Kinder und Jugendliche Knochen, Gelenke, Muskulatur
Knochen, Gelenke, Muskulatur Kopf, Nervensystem
Kopf, Nervensystem Lymphatisches System
Lymphatisches System Blase, Niere, Prostata
Blase, Niere, Prostata Psyche
Psyche Unfall
Unfall Verdauungsorgane
Verdauungsorgane Zähne, Kiefer, Mund
Zähne, Kiefer, Mund

Finden Sie die passende Klinik
In unserer Einrichtungs-Übersicht zeigen wir Ihnen, welche unserer Kliniken oder welches unserer Zentren und Institute Ihr Krankheitsbild behandelt.
Sie haben einen Termin in einer unserer Ambulanzen vereinbart? Hier finden Sie eine Übersicht unserer Ambulanzen mit Standort, Anmeldung und mitzubringenden Unterlagen.
Stationäre
Fälle
Ambulante
Besuche
Betten
Mitarbeitende
Universitätsmedizin Münster
Wir gestalten die Zukunft der Medizin zum Wohl unserer Patient*innen – durch Spitzenforschung, exzellente Lehre und modernste Krankenversorgung.

Krankenversorgung | Das UKM steht für Spitzenmedizin in der deutschen Krankenhauslandschaft.

Forschung | Wir forschen für die stetige Weiterentwicklung in der Krankenversorgung.

Lehre | Zusammen mit der Medizinischen Fakultät der Universität Münster bilden wir Ärzt*innen aus.
UKM-SOCIAL-WALL

Für Patient*innen
Informationen rund um ambulante Behandlung, stationären Aufenthalt und Besuch von Angehörigen

Für Zuweisende
Sie möchten eine Patientin oder einen Patienten in unsere Kliniken einweisen?

Karriere am UKM
Egal ob in der Pflege, im ärztlichen Bereich, in der Verwaltung oder Forschung: Wir sind immer auf der Suche nach neuen Kolleg*innen, die mit Begeisterung und neuen Ideen etwas Besonderes leisten und erleben wollen.